GERD Reflux after Sleeve Gastrectomy: Effective solution with Conversion to Gastric Bypass
The estimated number of Gastric Sleeve or Sleeve Gastrectomies performed annually in the USA is about 150,000. This effective bariatric procedure is among the least invasive physiologically since it is not associated with malabsorptive component. However, this procedure might not be perfect for everybody. One of the most frequent side effects is reflux of gastric contents into the esophagus associated with heartburn, regurgitation with sour tasting fluid coming up, chronic cough, throat burning or lumpy sensation in the chest or throat.
About 20-30% of patients might experience these symptoms after Sleeve Gastrectomy and for 5-10% symptoms are really bothersome to the point that surgery might be needed to control GERD. Often this is associated with weight regain due to maladaptive eating behavior since patients are trying to buffer the acid with foods.
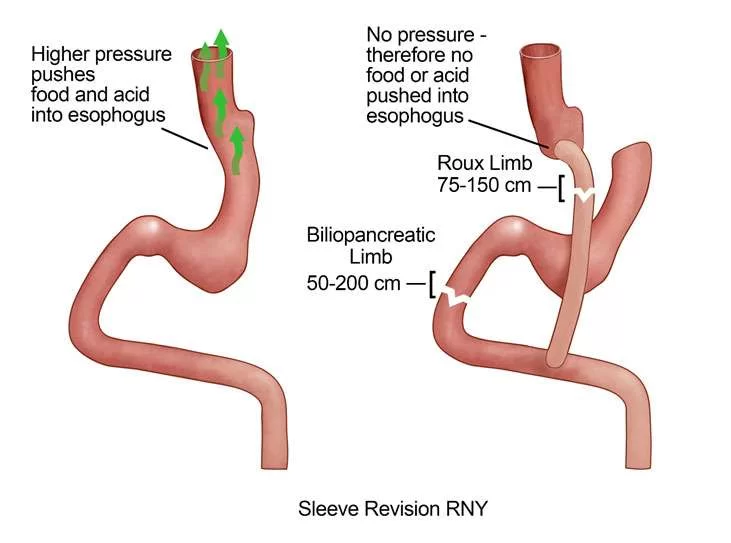
If conservative measures like acid reducing medications, avoidance of deep fried foods, acidic juices, soft drinks, certain fruits and caffeine do not work, patients should consider surgical treatment – Sleeve conversion to Gastric Bypass frequently with Hiatal hernia repair.
There are number of potential causes for development of significant GERD after a Sleeve surgery:
- Performing primary Sleeve Gastrectomy on patients with significant GERD, large Hiatal hernia, bile reflux
- Sleeve herniation into the chest later on after surgery with development of large Hiatal hernia
- Abnormal movement of the esophagus, a dysmotility that is exacerbated after surgery
- Incompetent valve mechanism of the esophago-gastric junction
- Sleeve stricture or narrowing by the scar tissue with angulation or twisting of the Sleeve
- So called “retained fundus” or excessive portion of stomach in the proximal part of Sleeve gastric tube
- Bile reflux
- Pressure gradient between narrowed stomach and esophagus with incompetent valve mechanism

All three surgeons were named
Top Docs 2022 in peer review
by “Baltimore Magazine”
-
Highest Ranking by Patients in Maryland
-
MBSAQIP National Accreditation
-
All major insurances accepted
-
Most major commercial plans are accepted
- Rated as Top Docs in 2022 by referring physicians
-
“Exemplary” designation from MBSAQIP
Surgical considerations
Before any surgery, substantially higher proportion of obese patients experience GERD compared to non-obese patients. Gastric Bypass with/without simultaneous repair of Hiatal hernia is considered the best surgical option for morbidly obese patients with GERD. With choosing Sleeve as an initial bariatric procedure for these patients, some surgeons were expecting for the GERD to get better with time after surgery and weight loss. The issue is that obese patients have abdominal “hypertension” or increased pressure inside the abdomen squeezing gastric contents into the esophagus. The popularity of Sleeve surgery among some surgeons was also driven by simplicity and expected absence of negative side effects.
With experience and acquisition of long-term follow up results, bariatric surgeons realized that we need to be careful when establishing indications for procedures and look for signs of GERD before surgery. As such Gastric Bypass is a better option for patients with significant reflux before surgery.
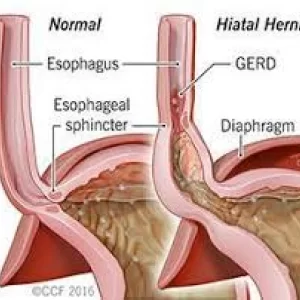
When Sleeve is converted to Gastric Bypass, surgeons are reducing the acid producing part of the stomach by 2/3 by creating a small bowel shunt or bypass. Reduced amount of acid and prevention of bile reflux into esophagus relieves the symptoms of heartburn and regurgitation. Also, repair of hiatal hernia (protrusion of the stomach into the chest that disrupts the valve mechanism of the junction) further facilitates symptom resolution by partially/completely restoring normal one-way valve mechanism of the esophago-gastric junction.
It has become apparent now that converting Sleeve Gastrectomy to Gastric Bypass is the only available meaningful option for patients with severe, troublesome GERD. A majority of patients (80-95%) notice nearly immediate resolution of reflux when conversion to Gastric Bypass is done simultaneously with Hiatal hernia repair. Even for those with persistent heartburn, symptoms are mild and easily controllable with acid suppressing medications.

With proper education with a dietician and regular follow up, Sleeve conversion to Gastric Bypass is associated with additional weight loss and improved quality of life. When deciding to have this operation, we encourage you to evaluate how severe your reflux symptoms are, effectiveness of medication and how much these issues are impacting your life.
Another consideration is that if patients develop GERD complications like esophageal ulcers or erosive esophagitis, strictures or Barret’s esophagus (that can increase the risk of esophageal cancer) surgery might be the only answer.
There is a misconception that Gastric Bypass surgery is automatically too complicated. Obviously, when considering Sleeve conversion to Gastric Bypass, you would like to consult surgeons who are performing this procedure frequently, possess substantial experience and have demonstrated good outcomes. You would like to look for such surgery to be performed at the fully credentialed bariatric surgery center to ensure best outcomes.
At the Ascension Saint Agnes Hospital, Certified Comprehensive Bariatric Surgery Program (accredited by MBSAQIP program of the ACS/ASMBS), our multidisciplinary team takes surgical, medical, dietary and behavioral factors into account to create an individualized plan of care for each patient aiming for the best possible results.
Bottomline: If you have severe, disabling GERD after Sleeve Gastrectomy with or without weight regain with proper workup and preparation conversion to Gastric Bypass with/without Hiatal hernia repair is the best and safe treatment option.
Request a Consultation Today!
